- 免费超放心报价
- 免费超放心量房
- 免费专车接驾
科技赋能,为您解放装修全过程
10分钟出报价 | 2小时出方案 | 24小时开工 | 45日交付
- 包施工 五星工长 10年以上经验
- 包主材 一线大牌+ 个性高级定制
- 包辅料 国际一线品牌 用料有保障
- 包售后 10年质保 终身维保
数装案例实录
国际大师设计1:1复制到您家,用10W+案例助您找到装修灵感查看更多实景案例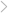
- 现代简约
- 北欧
- 新中式
- 现代轻奢
- 新古典
- 混搭
 #全景案例
#全景案例
-

180平米3室2厅1厨2卫户型现代简约装修风格案例
现代简约 三居室 | 180㎡
-

220m²现代简约装修,简洁有品位,高级又舒适!
现代简约 普通住宅 | 220㎡
-

东源阅境330平米现代简约风格装修设计效果图
现代简约 四居室 | 330㎡
-

雁栖半岛600平现代简约装修效果图
现代简约 普通住宅 | 600㎡
-

155平北欧风格两居室装修效果图
北欧 普通住宅 | 155㎡
-

江山樾 245㎡ 北欧装修 装修设计案例
北欧 普通住宅 | 245㎡
-

格调林泉 欧式风格
北欧 三居室 | 180㎡
-

陆港金海岸 北欧风格装修效果图 280平米 五室两厅
北欧 普通住宅 | 280㎡
-

英伦庄园388平米新中式风格装修设计效果图
新中式 四居室 | 388㎡
-

紫禁长安 新中式风格装修效果图 223平米 四室三厅
新中式 普通住宅 | 223㎡
-

生活的诗意藏于点滴,480平方现代+新中式装修
新中式 平层 | 480㎡
-

逸翠尚府 混搭风格装修效果图 198平米 三室两厅/三居室
新中式 三居室 | 198㎡
-

禹洲雍贤府200平三居室现代轻奢风装修设计案例
现代轻奢 三居室 | 200㎡
-

随州四季花园220平米现代轻奢风格装修效果图
现代轻奢 普通住宅 | 220㎡
-

1000平米现代轻奢风装修效果图
现代轻奢 复式 | 1000㎡
-

理想的家 美式轻奢,不仅是风格更是生活
美式 普通住宅 | 500㎡
热装楼盘
500+超放心在施工地,总有一个在您身边看看我家旁边的在施工地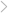
29座城市46家线下体验店
50万用户口碑推荐,无论您在哪里,东易日盛都在您身边
客户评价
好不好业主说了算,真实案例效果看了才放心更多用户评价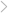


装修流程
-
线上预约
-
看样板间
-
规划新家
-
签订合同
-
如期开工
-
竣工验收
-
售后保障
超放心数装服务 让装修不再操碎心
7大超放心家装品质系统,用实力让家美好呈现
-

超放心量房 32种神器精准量房
免费上门到家 -

超放心报价 建筑级精准报价神器
精准到家 -

超放心设计 大师领衔设计
1:1还原到家 -

超放心选材 国际一线大牌
严选标配到家 -

超放心工艺 欧系八大工艺
金牌工人落地到家 -

超放心交付 从施工到交付不操心
全程透明省心到家 -

超放心售后 10年质保入合同
售后无忧到家
超放心装修小课堂
- 装修前
- 装修中
- 装修后
- 装修问答
#本月热门小课堂
对装修不太懂的小伙伴儿来说装修是一大难题,看看本月装修热门内容全解析,小白也能轻松装~
-
【房产】绿色家装:创造健康与舒适的生活空间
绿色家装比起普通的家装,它提高人们生活质量,保护人们身体健康,创造绿色健康的家居环境。绿色家装是现在更受大家欢迎的一种家装方案。它主要包含了以下几个方面:1,尽量用绿色环保材料。2,考虑使用节能电器。3,施工时要严格按照环保标准施工。4,做好室内环境检测。
2024/01/15 09:52:32 -
【预算】绿色家装贵不贵?绿色家装成本解析!
随着环保意识的日益增强,绿色家装成为越来越多人的选择。那么绿色家装的成本是一个关键的考虑因素。绿色家装到底贵不贵?我们通过1.材料成本,2.施工成本,3.时间成本三个方面来探讨这个问题的答案。
2024/01/15 09:52:17 -
【预算】旧房翻新装修价格:从预算到实现的全面规划
旧房翻新改造是一项复杂的工程,涉及到多个环节和预算的考虑。从拆改到水电工程,再到墙面处理,每一步都与费用息息相关。但是很多人对旧房翻新装修价格是完全没概念的。其实旧房翻新装修价格主要要看这几方面:1,拆改费用。2,水电工程费用。3,地板砖费用。4,墙面费用。5,家具家电费用。
2024/01/15 09:52:02 -
【房产】老房翻新设计:让老房焕发新生
随着时间的推移,许多老房渐渐的失去了以往的光彩,变得老旧。然而,通过精心老房翻新设计和改造,这些老房可以焕发新生,成为舒适、时尚的居住空间。对于老房翻新设计的关键点,我相信很多网友都是非常感兴趣的,他主要有这4点:1,对房屋进行全面评估。2,业主和设计师沟通后制定详细的设计方案。3,关注细节地方。4,合理安排施工流程。
2024/01/15 09:51:51
-
【拆改】房屋装修结构拆改注意事项 承重墙常见误区介绍
当我们在装修房屋的时候,很多人都会通过主体拆改或更改房屋结构来让房屋变得更加宽敞,那么房屋装修结构拆改注意事项都有哪些呢?在进行拆改的时候,这些注意事项一定要铭记在心,如果我们没有注意到这些问题,可能装修出的效果并不能令我们满意。
2020/11/02 18:25:10 -
【拆改】什么是装修主体拆改 主体拆改要注意什么
我们在对新房进行装修的时候,难免会根据居住者的居住习惯来对房屋的墙面进行拆改,一是为了方便居住者的日常起居,二是为了提高室内的美观性。但是很多朋友可能并不知道什么是装修主体拆改,更加不知道在进行主体拆改的时候应该注意什么。对于
2020/11/02 18:24:55 -
【拆改】怎么安全拆墙 安全拆墙的方法有哪些
房屋拆墙是必须要做的一件事,如果我们盲目的进行房屋拆改,施工的过程中可能会发生安全隐患,那么我们应该怎么安全拆墙呢?本文内容将会围绕着这个问题展开详细的介绍
2020/11/02 18:24:44 -
【拆改】装修哪些墙可以拆 拆墙需要注意什么
房屋装修中,拆墙是必不可少的,也是装修中最为重要的一个步骤,拆墙能够让我们的房屋变得更加宽敞,方便我们的生活,那么拆墙需要注意什么呢?这个问题小编将会从下文中为大家详细的介绍一下这个问题。
2020/11/02 18:24:31
-
【软装】南京装修预算怎么分配?如何在预算内打造6种舒服阅读角落?
舒适、温馨、极度放松的完美阅读角落,可说是开启一段书中冒险的大门。虽然随处都可以成为你的阅读空间,但最好的阅读角落还是必须根据个人喜好及人们阅读时感到舒适的关键因素而打造而成。如果您想要重新改造阅读角落,这里有一些简易又实用的改造想法,让您了解如何在装修预算内及快速营造出舒适阅读角落。
2021/06/10 13:27:55 -
【入住】冲破行业低迷,看东易日盛超放心家装如何逆势生长
东易日盛提出了超放心品质系统这一理念。即超放心量房、超放心报价、超放心设计、超放心选材、超放心工艺、超放心交付、超放心售后,几乎每项都是针对行业乱象和客户痛点提出的解决办法。
2021/03/10 16:41:25 -
【入住】您有一份《东易日盛超放心家装升级宝典》,请查收
2021牛年就这样拉开了大幕,怀着对新年新生活的期待,我们度过了近几年最让人难忘的一次春节假期。去年的鼠年对每个人来说都算不上那么美好,疫情的暴发迅速改变了人们的生活和工作习惯。2020年的经历让核酸检测成了热词,也让口罩变成了出门必带单品,虽然2021年依旧充满着许多不确定性,不知道疫情会不会卷土重来,不知道经济能否触底反弹,但相信2021年人们一定可以将一切不确定变得很确定,让一切不放心变得超放心。
2021/03/10 16:39:12 -
【入住】24年如一日,东易日盛超放心家装视交付为根本
经历了2020年疫情的冲击后,家装市场的竞争愈发激烈,很多中小体量的家装公司因资金链或施工售后等种种原因,已逐渐被市场所淘汰,在这样的“乱世”之下,像东易日盛超放心家装这样的很多大装企反而迎来了一波业绩的增长。
2021/03/10 16:30:26
-
装修公司选择有何注意事项
现如今家装公司比较多样化,整个行业也比较混乱,难免会有不正规的公司存在其中。为了可以给业主提供优质的家装设计服务,大家还是要仔细认真挑选专业并且可靠的装修公司。对于没有经验的新手来说,在挑选装修公司时,必须要注意:1、确定装饰公司的资历;2、与装饰公司初步接洽;3、确定公司售后服务这些小细节,这样才可有效避免选择过程中犯错误。
2023/11/23 09:01:23 -
装修找哪家装饰公司好
面对家装这个事情时,很多业主时常会觉得十分困扰。毕竟,国内的整个家装行业比较混杂,大大小小的公司云集了不少,这才导致了大家时常会为装修找哪家装饰公司这个问题而感到困扰。通过不断的总结,发现东易数装是众多的公司当中比较不错的一家,这家公司的主要优势有:1、注重个性化定制;2、强调品质与可靠性;3、注重打造环保家居空间;4、提供良好的售后服务这几点,大家了解过后,可以确定是否选择。
2023/11/21 13:11:08 -
装修前验房步骤有哪些
在收到了开发商提供的收房通知之后,业主要及时的对即将收入手的房子进行验收。这也是大家在开始装修设计新房子之前,必须要经历的一个环节。很多人虽然知道有这样一个环节,但是却不知道具体应该怎么去做。事实上,装修前验房步骤当中比较重要的有:1、仔细核对装修材料是否有误;2、门的验收;3、电路验收;4、水路验收这四个步骤,大家还是要引起重视,然后一步步的去操作。
2023/11/21 17:47:11
20余年 50万+中国家庭 100+城市 装修经验沉淀
东易日盛家居装饰集团全资子公司
共享上市公司20余年供应链 、工艺、全屋定制 和集团管控六大优势
基于科技赋能和大牌用料与空间收纳扩容 解决居住难题
为经济适用人群装修一个好而不贵的家,让居住更省心,生活更放心

-
46家
线下体验店 -
30+
城市覆盖 -
4000+
资深服务团队 -
7*24小时
为您守候




 装修前
装修前 装修中
装修中 装修后
装修后 装修问答
装修问答 品牌介绍
品牌介绍 品质联盟
品质联盟 客户口碑
客户口碑 东易日盛旗下数装产品
东易日盛旗下数装产品
 科技化家装理念
科技化家装理念
 颜值+品质全满足
颜值+品质全满足
 超放心售后保障
超放心售后保障
 家装行业A股上市
家装行业A股上市
















 三居室
三居室
 竣工
竣工
 105㎡
105㎡
 10255次
10255次






















































